Author's personal copy
LETTER TO THE EDITOR
Prenatal Ultrasound and Magnetic Resonance
Imaging Findings of Fetal Akinesia Deformation
Sequence with Multiple Pterygium Syndrome
Chih-Ping Chen
1,2,3,4,5,6,7*
, Jin-Chung Shih
8, Chen-Yu Chen
2,
Schu-Rern Chern
3, Jun-Wei Su
2,9, Wayseen Wang
3,101Department of Medicine, Mackay Medical College, New Taipei City,2Department of Obstetrics and Gynecology, Mackay Memorial Hospital,3Department of Medical Research, Mackay Memorial Hospital, Taipei,4Department of Biotechnology, Asia University,5School of Chinese Medicine, College of Chinese Medicine, China Medical University, Taichung,6Institute of Clinical and Community Health Nursing, National Yang-Ming University,7Department of Obstetrics and Gynecology, School of Medicine, National Yang-Ming University,8Department of Obstetrics and Gynecology, National Taiwan University Hospital, Taipei,9Department of Obstetrics and Gynecology, China Medical University Hospital, Taichung, and10Department of Bioengineering, Tatung University, Taipei, Taiwan
Received 10 February, 2012; accepted 15 February, 2012
A woman aged 27 years, gravida 2, para 1, was referred for genetic counseling at 27 weeks of gestation because of reduced fetal movement, scoliosis, and clubfoot detected by ultrasonography. She and her husband were non-consanguineous and healthy and had a son aged 3 years. The woman did not abuse drugs, and she did not have any metabolic conditions or neuromuscular disorders, such as myasthenia gravis, during this pregnancy. Amniocentesis revealed a karyotype of 46,XY, and array comparative genomic hybridization analysis revealed no genomic imbalance. A level 2 ultrasound at 29 weeks of gestation revealed a singleton male fetus with fetal biometry equiv-alent to 29 weeks, reduced fetal movement, severe kyphoscoliosis, pulmonary hypoplasia, and arthrogryposis
(Fig. 1). Magnetic resonance imaging (MRI) study addition-ally showed multiple pterygia (Fig. 2). The fetus had intrauterine fetal death, and a 1234-g fetus was delivered with down-slanting palpebral fissures, hypertelorism, a depressed nasal bridge, low-set ears, micrognathia, joint contractures, and multiple pterygia (Fig. 3). Radiographic studies showed kyphoscoliosis and a restrictive left chest (Fig. 4). Molecular analysis revealed no mutation in the genes of CHRNA1, CHRND, CHRNG, RAPSN, or DOK7.
Fetal akinesia deformation sequence (FADS) is a clinically and genetically heterogeneous disorder that is characterized by fetal akinesia, arthrogryposis, intrauterine growth restriction, congenital abnormalities, such as cystic hygroma, pulmonary hypoplasia, facial cleft, cardiac defects, cryptorchidism, and intestinal malrotation, and occasionally pterygia of the limbs [1]. The incidence of FADS is about 1:15,000 births[2]. FADS may phenotypically overlap with the lethal type of multiple pterygium syndrome (LMPS). FADS/LMPS can be caused by neuropathy, muscular disorders, neuromuscular junction disorders, myasthenia
* Correspondence to: Dr Chih-Ping Chen, Department of Obstet-rics and Gynecology, Mackay Memorial Hospital, 92, Section 2, Chung-Shan North Road, Taipei, Taiwan.
E-mail address:cpc_mmh@yahoo.com(C.-P. Chen).
0929-6441/$36ª 2012, Elsevier Taiwan LLC and the Chinese Taipei Society of Ultrasound in Medicine. All rights reserved. doi:10.1016/j.jmu.2012.02.002
Available online atwww.sciencedirect.com
journal homepage: www. jmu-online .com Journal of Medical Ultrasound (2012) 20, 61e63
Author's personal copy
Fig. 1 Prenatal (A) two-dimensional; and (B) three-dimensional ultrasound demonstration of kyphoscoliosis.
Fig. 2 Magnetic resonance imaging of the fetus shows (A) webbing of the neck (arrows); (B) pterygia with fixed deformity of the elbow (arrow); (C) pterygia with fixed deformity of the left lower limb (arrow).
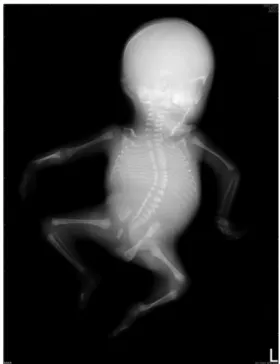
Fig. 3 Fetus at birth. Fig. 4 Radiography shows severe kyphoscoliosis.
Author's personal copy
gravis, restrictive dermopathy, in utero restriction space of the fetus, vascular compromise, ischemia, teratogenic exposures, circulating maternal antibodies to neurotrans-mitters, myelin, and muscle proteins [1,3,4]. Prenatal ultrasonography findings of FADS/LMPS include lack of extremity motions, persistent abnormal limb posture, poly-hydramnios, pulmonary hypoplasia, a short umbilical cord, increased nuchal translucency, cystic hygroma, and hydrops fetalis [5,6]. Fetal MRI has been suggested as a useful adjunct to ultrasound in evaluating associated central nervous system abnormalities [6,7]. Prenatal diagnosis of FADS/LMPS should include a differential diagnosis of spina bifida, trisomy 18, fetal constraint, body stalk anomaly, caudal regression sequence, fetal hypoxia, amniotic band sequence, fetal neck masses, joint and vertebral anomalies, and iniencephaly[8].
Acknowledgments
This work was supported by research grants NSC-97-2314-B-195-006-MY3 and NSC-99-2628-B-195-001-MY3 from the National Science Council, and MMH-E-100-04 from Mackay Memorial Hospital in Taipei, Taiwan.
References
[1] Vogt J, Morgan NV, Marton T, et al. Germline mutation in DOK7 associated with fetal akinesia deformation sequence. J Med Genet 2009;46:338e40.
[2] Bayat A, Petersen A, Møller M, et al. Incidence of fetal akinesia-hypokinesia deformation sequence: a population-based study. Acta Paediatr 2009;98:3e4.
[3] Ravenscroft G, Sollis E, Charles AK, et al. Fetal akinesia: review of the genetics of the neuromuscular causes. J Med Genet 2011;48:793e801.
[4] Rink BD. Arthrogryposis: a review and approach to prenatal diagnosis. Obstet Gynecol Surv 2011;66:369e77.
[5] Gupta P, Sharma JB, Sharma R, et al. Antenatal ultrasound and MRI findings of Pena-Shokeir syndrome. Arch Gynecol Obstet 2011;283(Suppl. 1):27e9.
[6] Nemec SF, Hoftberger R, Nemec U, et al. Fetal akinesia and associated abnormalities on prenatal MRI. Prenat Diagn 2011; 31:484e90.
[7] Senocak EU, Oguz KK, Haliloglu G, et al. Prenatal diagnosis of Pena-Shokeir syndrome phenotype by ultrasonography and MR imaging. Pediatr Radiol 2009;39:377e80.
[8] Byrne JLB. 7 Musculoskeletal: abnormal fetal posture/move-ment. In: Woodward PJ, Kennedy A, Sohaey R, Byrne JLB, Oh KY, Puchalski MD, editors. Expert ddx: obstetrics. 1st ed. Salt Lake City, UT: Amirsys Inc; 2009. p. 2e7.